Medically reviewed by Laurie Marbas, MD
When my dad was growing up as the presumed heir to the Baskin-Robbins company (before he left all the ice cream and all the wealth to follow his own “rocky road”), he had an ice cream cone-shaped swimming pool in his backyard. Surrounded by shade trees, the pool was an inviting and cool oasis during the hot California summers.
And while the hero of the story appears to be the ice cream empire that paid for the pool and inspired its shape, what really made those swims safe and enjoyable was the humble pool filter.
Without the filter’s constant diligence, the water would quickly have turned murky, smelly, and unsafe. An aerial photo of the backyard shows the pool itself, a lawn, and a patio — but no pump or filter. These unglamorous elements were hidden out of sight, and not given a second thought as long as they did their job.
Which brings me to today’s topic — the kidneys. They act as filters in our bodies, cleansing the blood, removing waste, and keeping our fluids in a healthy balance. They also perform some amazing and crucial tasks as part of the endocrine system (which is where the pool filter analogy falls short).
Also unlike pool filters, it’s not immediately obvious when the kidneys begin to fail. While in the US, 1 in 7 people have chronic kidney disease, and globally that figure is about 1 in 10, the majority don’t even know they have it. That’s because the disease may not cause any symptoms until it reaches an advanced stage, at which point it often becomes life-threatening in a hurry. And kidney disease incidence is on the rise, largely because of lifestyle and dietary changes that have increased its prevalence, as they have with so many other non-communicable, chronic diseases.
In this article, we’ll explore how chronic kidney disease (CKD) develops, and what it does to our bodies. We’ll also look at lifestyle factors that contribute to CKD, with a particular focus on foods for kidney health (those that can help or harm kidney function). And we’ll finish up with some yummy recipes that your mouth and kidneys will love.
What are the Functions of the Kidneys?
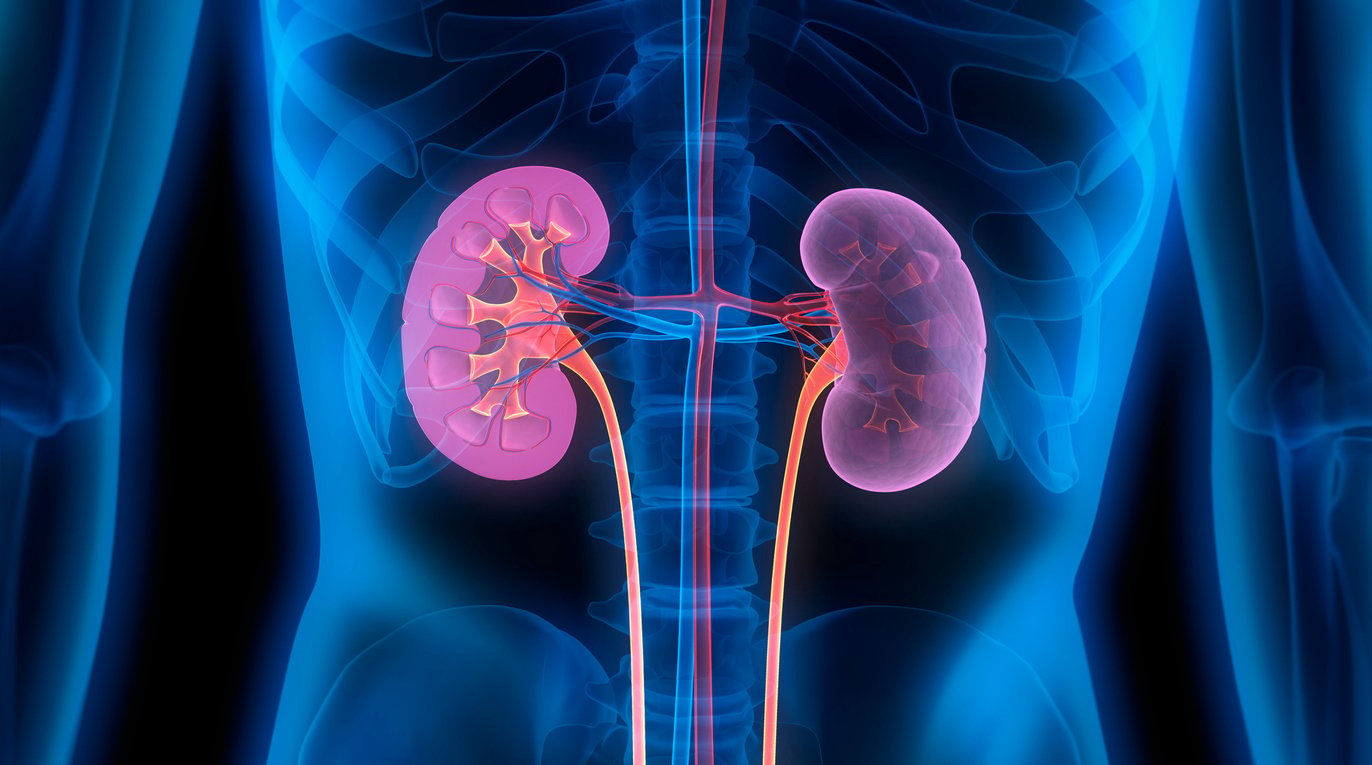
While the kidneys are famous for removing waste and excess fluids from the body — as well as inspiring the shape of some swimming pools and the name of the widely consumed kidney bean — they do so much more. Before we get to those functions, let’s locate them in the body.
The kidneys are a pair of organs, each about the size of a fist, located on either side of the spine just below the floating ribs. As part of the urinary system, the kidneys excrete urea (made by the liver as a byproduct of protein metabolism), which is a major component of urine. Unlike sugars and fats, the body has no means of storing proteins for later use, so the excess has to be excreted to prevent toxic buildup.
In addition to secreting urea, the kidneys remove other waste products, such as drugs and other foreign chemicals, that aren’t native to the body. They also get rid of excess fluid and regulate the fluid-electrolyte balance in your body by continuously filtering your blood.
And by “continuously,” I do mean continuously. The kidneys filter about 200 quarts of fluid every 24 hours. The average adult has about five quarts of blood, which means that every drop of blood takes a ride through these organs around 40 times per day. (Forget Space Mountain, the most amazing ride can be found in Kidneyland!)
Of those 200 quarts, about 198 are cleaned and returned to the body, good as new, while the remaining two or so quarts are excreted. That’s partially the basis for the often-stated recommendation to drink eight cups of water — two quarts — a day.
If I were writing an infomercial about the kidneys (“Act now, and get two for the price of one” — gosh, this practically writes itself), this is where I’d say, “But wait — there’s more.” The kidneys regulate bodily concentrations of sodium, potassium, and other vital minerals, as well as maintain exquisite control over your body’s acid content.
Kidney Hormones
Your kidneys do much more for you than you may have realized. Kidneys are also highly social organs that love to chat with their colleagues. They produce hormones that affect other organs. One of these hormones is renin, which the body uses to manage your blood pressure. The kidneys also make a chemical called erythropoietin, which prompts your body to make new red blood cells. (A synthetic version of this chemical given to advanced CKD sufferers is also a popular doping agent used by athletes who want to improve their cardiovascular efficiency.)
The kidneys also convert vitamin D3 — which you either get in supplement form or metabolize from sunlight on your skin — into the active form of vitamin D (known to its many chemistry buff fans as 1,25-dihydroxycholecalciferol) that supports the immune system, strong skin and bones, and many other vital functions.
How Does Chronic Kidney Disease Happen?
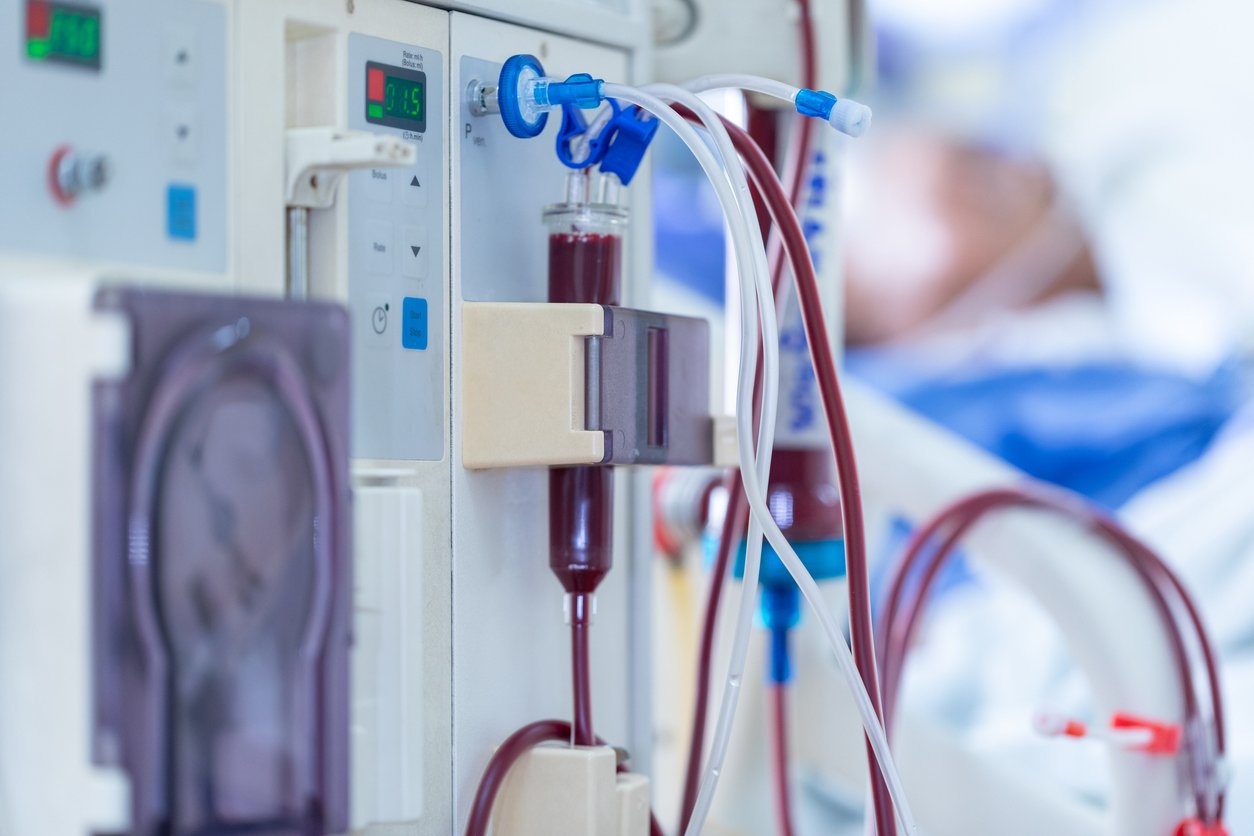
Chronic kidney disease, the most common condition involving the kidneys, develops over time when the organs are damaged, most often as a result of diabetes and hypertension. It’s a sneakily gradual loss of kidney function, very different from acute renal injury. (“Renal” comes from the Latin word for kidney. Confusingly, a kidney doctor is called a “nephrologist,” from the Greek for kidney, “nephros.”) Acute renal injury, in which the kidneys suddenly stop working, can occur in a matter of days or hours.
In CKD, the kidneys have been structurally and/or functionally abnormal for at least three months, and aren’t able to filter blood properly. As the damage increases, patients move through a number of stages until, in the last one, stage 5, kidneys are functioning at less than 15% of their normal capacity. This is the cutoff for the clinical definition of renal failure.
At that point, known as end-stage renal disease (because a patient doesn’t typically recover from it), dangerous levels of fluid, electrolytes, and wastes can build up in the body. To stay alive, a patient will need dialysis or a kidney transplant. Dialysis, which is the mechanical filtering of blood either inside or outside the body, can replace the kidney’s filtering process to some extent but it doesn’t address the signaling functions or the vitamin D conversion that the kidneys can no longer perform.
When the kidneys fail, the rest of the body suffers. CKD can increase the risks of overaccumulation of fluid in the lungs, malnutrition, heart disease, weak bones, and a dysregulated immune system.
The kidneys don’t decide one day to go on strike — the road from healthy to “we’re outta here” typically takes years, if not decades. While genetics may play a role in CKD, lifestyle factors such as elevated blood sugars, high blood pressure, smoking, and high cholesterol also increase the risk of developing CKD. And the longer you expose your body to those factors, the more likely your kidneys are to lose function.
The Type 1 and Type 2 Diabetes Connection

Approximately 40% of patients with type 1 diabetes and 30% of those with type 2 diabetes may eventually suffer from CKD. This occurs because diabetes damages the small blood vessels of the kidney, decreasing its ability to filter the blood.
Impaired blood filtration brings a few consequences. First, fluid retention in the body can occur, resulting in edema, or swelling, typically in the arms and legs. (If you’re a fan of 19th century English literature, you may have come across its archaic name, “dropsy,” which really paints a mental picture.) Kidneys can also lose protein — it leaks from the kidneys into the urine. Finally, the level of waste products in the blood can increase.
Diabetes also causes bladder dysfunction, including decreased bladder sensation and impaired bladder emptying, which increases the risk of infection. Diabetic neuropathy (nerve damage) can wreak further havoc by making it hard to empty the bladder, or even feel when the bladder is full. And the pressure from an overfull bladder can cause pressure to build in the kidneys themselves, causing further injury. (That advice from your grandma to “never hold it in” turns out to be right on.)
Plus, if urine that is high in sugar stays in the bladder for too long, an infection may develop from the rapid growth of bacteria in that sugar-rich environment.
Learn what the latest scientific research says about how to prevent and reverse type 2 diabetes — using food and free lifestyle tips.
Join the FREE

Watch Here
High Blood Pressure and Kidney Disease

High blood pressure, or hypertension, can also damage blood vessels in the kidneys. Because hypertension makes the heart work harder to pump blood, pressure on the kidney walls increases. This pressure can compromise the efficiency with which they remove waste and extra fluids. Now we’ve got a vicious cycle between hypertension and kidney disease, in which those excess fluids further raise blood pressure, which makes the kidneys even less efficient.
Diagnosing Chronic Kidney Disease & Dysfunction
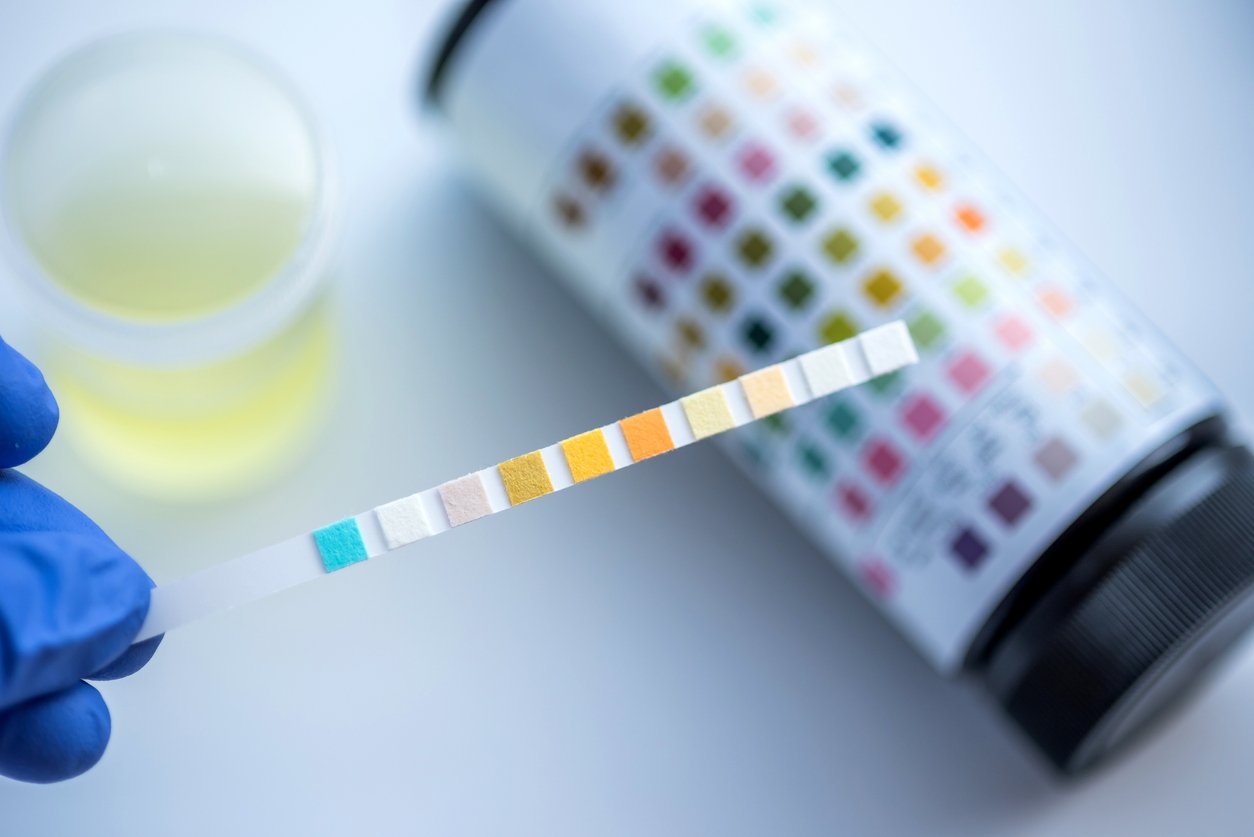
Since you can suffer from progressive CKD long before it causes clinical problems, it’s important for those at risk (i.e., already having high blood pressure, diabetes, heart disease, or a family history of kidney disease) to monitor the status of their kidney health. There are several ways to do this.
Blood tests can check how well your kidneys are filtering your blood. The most common metric for kidney function tests is the glomerular filtration rate (GFR). GFR can be calculated using serum creatinine and is inversely related, meaning the higher the creatinine the lower the GFR.
A comprehensive metabolic panel, or CMP blood test, often includes a kidney function test, namely, testing for GFR. While you can go through a health care provider to get this standard blood testing done, you can also order at-home kidney function tests, which include the CMP. Check out our article on ordering your own lab tests.
Another marker for kidney disease severity used in kidney function tests is urine albumin, which has nothing to do with the headmaster in Harry Potter. Albumin is found in the blood, is important for fluid homeostasis, and transports hormones, vitamins, and enzymes throughout the body. When there is albumin in the urine, it suggests there may have been damage to the kidneys’ filtering system.
Imaging may be helpful to further evaluate kidney function if needed, including kidney structure and assessing blood flow. In some cases, a kidney biopsy may be necessary to further diagnose the cause of kidney dysfunction.
Lifestyle Changes for Chronic Kidney Disease
Because of the association with type 2 diabetes and high blood pressure, which have a strong link to diet and lifestyle, there are some important things people can do to help prevent the development and slow the progression of CKD. Here are some of the most important ones.
Exercise and Kidney Function

Not being physically active is both a contributing factor for and consequence of kidney disease. By the time someone is on dialysis, they may not feel like moving around much. Their increasingly sedentary lifestyle is associated with an increased risk of additional diseases and premature death.
Research shows that adding gentle exercise can help people at all stages of CKD, and lower the risks of comorbidity, hospitalization, and mortality while enhancing the quality of life.
Kidneys and Smoking
This piece of advice could fit into just about any article on health. For most people, quitting smoking will have a tremendous positive impact on all health outcomes, including kidney disease.
Maintain a Healthy Weight

Obesity is one of the risk factors most predictive of CKD onset. Ironically, the disease itself can lead to significant weight loss, as CKD can cause loss of muscle mass (and strength) as it progresses. When weight loss in CKD patients occurs, they may need to focus on getting enough nutritionally dense calories to maintain a healthy weight.
Get Enough Sleep

Sleep affects all aspects of health. And it turns out that the kidneys operate on a time schedule, with certain functions regulated by the body’s circadian rhythm.
There are links between kidney disease and sleeplessness: an ongoing pattern of insufficient or disrupted sleep is associated with an increased risk of CKD. It’s common for CKD patients to struggle with sleep, which can worsen disease progression. If that’s you, put attention into improving your sleep through sleep hygiene, including creating an environment that’s conducive to deep sleep, and optimizing your diet and meal timing for sleep.
Reduce Stress Levels
Stress harms the body in many different ways, and the kidneys are no exception. Research has found an association between stress-related disorders and increased risk of both chronic and acute kidney disease. One 2018 study found that the more people worried about achieving their goals, the higher the rates of CKD. There are many effective ways to reduce chronic stress levels, including practicing mindfulness and other stress-reduction techniques, reducing stress-related triggers, setting realistic goals and expectations, and choosing a dietary pattern that supports balanced hormone levels. Speaking of which…
Eat a Healthy Diet

Although genetic factors play a role in kidney disease, the majority of cases are preventable. And a kidney healthy diet is probably the most important implement in the prevention toolbox. Researchers estimate that roughly one-quarter of CKD cases in industrialized countries can be attributed to nutritional factors — and this is likely a very conservative estimate.
As industrialized diet patterns have been directly implicated in the development of both type 2 diabetes and high blood pressure, it makes sense that what you eat can affect the development and progression of CKD, as well. Specifically, diets high in animal protein and low in fruits and vegetables have been associated with CKD. The best-odds, “happy kidney” diet consists largely of whole plants, with limited or no animal protein.
Renal Nutrition: Can a Plant-Based Diet Help?

Plant-based diets can decrease the incidence of cardiovascular disease, decrease rates of type 2 diabetes and obesity, and reduce inflammation and cholesterol. Since these outcomes may delay kidney failure and the initiation of dialysis, some clinicians look to plant-based diets as a strong contender to prevent and slow the progression of CKD.
An optimal renal diet emphasizes high-fiber and low-fat foods and, as I just mentioned, substantially reduces or (better yet) eliminates animal-derived protein. Here’s why this is so important: Increased fiber intake changes what the gut microbiota produce, lowering the amounts of uremic toxins. These toxins, which come from animal-based protein, take a heavy toll on the kidneys, which have to break them down, filter, and excrete them. The more fiber you eat, and the less animal protein, the fewer problems you’ll have with uremic and other toxins. Animal protein is no friend to your kidneys.
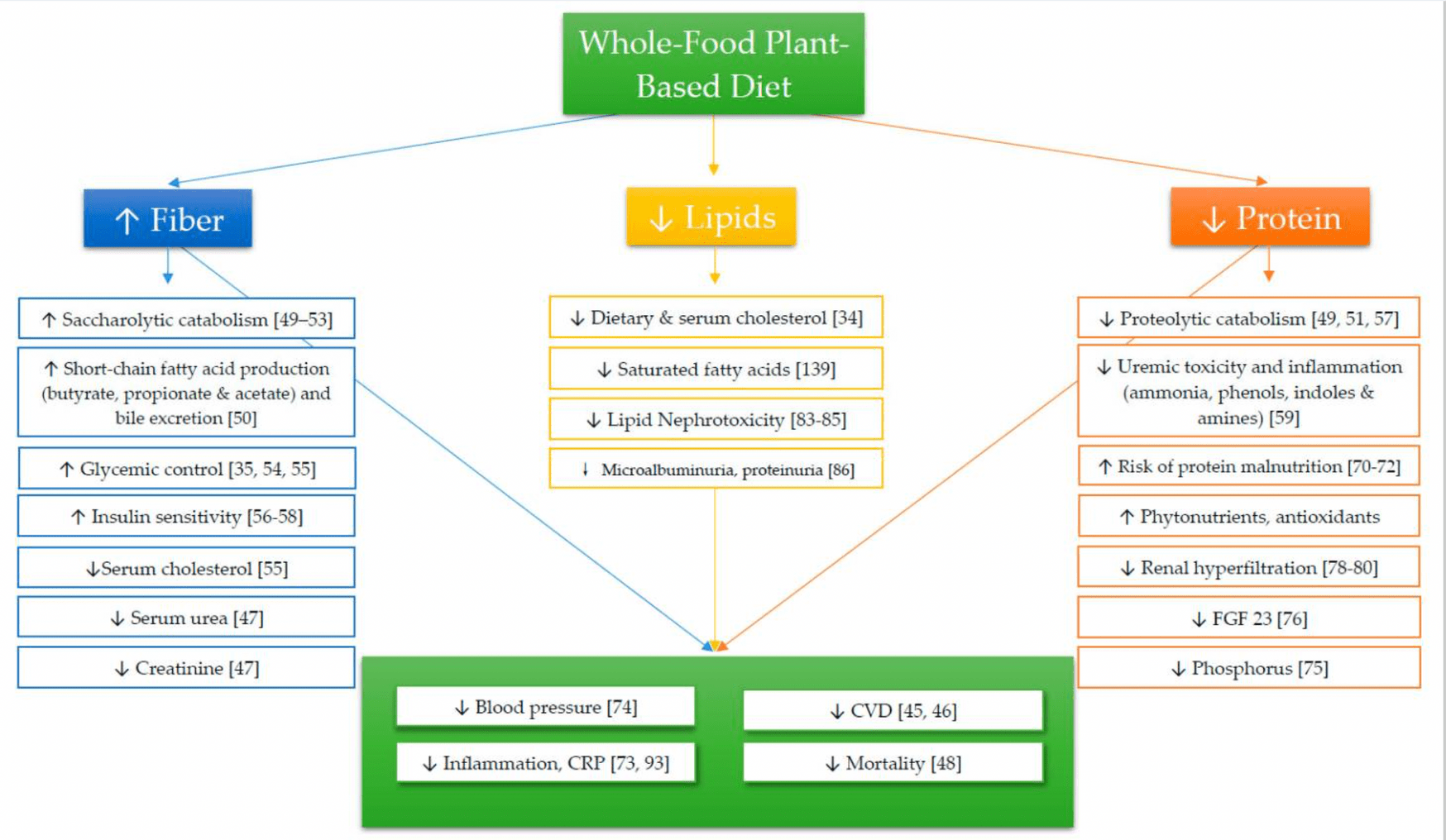
The figure above shows how these elements can work together to increase helpful compounds and decrease harmful ones to positively affect CKD outcomes.
One of the most impactful dietary changes you can make to keep your kidneys healthy is to swap animal protein with plant protein. This shift can protect you from a nasty — life-threatening, actually — condition called metabolic acidosis (an electrolyte disorder and complication of kidney disease) by lowering acid production in your body.
In a kidney-friendly diet, the dietary source of the protein may be of greater importance than the amount of protein, as plant-derived protein comes with many other beneficial components including fiber, antioxidants, and phytonutrients — all of which are good for kidney health.
Plant-sourced protein sources are also generally lower in saturated fat, and have no cholesterol, unlike animal foods whose dietary cholesterol and saturated fat have been linked with decreased insulin sensitivity, oxidative stress, high LDL cholesterol, and high blood pressure. In short, adopting a whole foods, plant-based diet has been shown to have numerous health benefits for the kidneys, many of which are clinically relevant for the management of CKD.
Other Nutrients That Need Monitoring in CKD
While simply eating more plants, fewer animals, and fewer highly processed foods can help manage CKD, there are some nutrients of concern that deserve special attention.
Phosphorous
One of these is phosphorus, which along with calcium helps build strong, healthy bones, and contributes to overall health. But it’s possible to have too much of a good thing — patients with CKD have trouble excreting excess phosphorus, which can actually weaken bones.
High phosphorus levels can also contribute to dangerous calcium deposits in your blood vessels, lungs, eyes, and heart. One way to avoid excess phosphorus, fortunately, is to limit animal protein, which has high concentrations of the nutrient. Another strategy is to avoid fast foods, sugar-sweetened beverages, and most packaged and processed foods, many of which contain phosphorus as an additive or preservative. Phosphorus from these sources is more readily absorbed by the body, making it especially harmful for people with CKD.
Sodium
Too much sodium in a person’s diet can be harmful because it causes blood to retain fluid. People with CKD need to be careful not to let too much fluid build up in their bodies, as we’ve seen.
CKD patients are often advised to follow the DASH (Dietary Approaches to Stop Hypertension) diet, which is prescribed to people with hypertension to lower their sodium intake. This diet is associated with a lower risk of end-stage kidney disease in individuals with CKD and high blood pressure.
Most sodium in the modern industrialized diet comes from processed, packaged, and fast foods, so it’s a good idea to limit or eliminate these foods if sodium is an issue for you.
Potassium
Potassium is another nutrient of concern. Hyperkalemia (too much potassium in the blood) is a severe metabolic condition that patients with CKD often experience. As kidney disease progresses, the kidneys’ ability to excrete potassium decreases.
Patients often receive advice to limit dietary potassium intake to maintain their serum potassium levels within the normal range. The benefits of restricting potassium in CKD patients aren’t settled science, however, given that a plant-based diet with a high content of potassium-rich foods can be beneficial and slow the progression of CKD. What most folks can agree on, however, is the benefit of testing for potassium levels, to ensure they are in the normal range.
Vitamin D
Vitamin D transforms in the kidneys into the form your body can use, and CKD can interfere with that process. Whether or not you have CKD, it’s best to get enough vitamin D, whether from your body’s response to the sun, or from a supplement. When your vitamin D levels are too low, you can also end up with low calcium levels. That’s because vitamin D helps your body absorb calcium.
Calcium
Calcium metabolism and regulation are complicated and compounded with CKD. Getting too much or too little can both be problematic. To be safe, it’s usually best to get calcium from food — as supplements could give your body too much and increase your risk of kidney stones.
Click here for more on calcium.
Oxalates
Oxalates are another compound found in certain foods that may cause calcium oxalate kidney stones, which can make CKD worse. They’re also involved in inflammatory pathways. So if you consume too many of them in your diet, that could contribute to the progression of CKD and systemic inflammation.
You can reduce the levels of oxalates in some high-oxalate foods by cooking them. Choosing foods that are high in calcium and magnesium and drinking water can help reduce the negative impact of oxalates.
Click here for more on oxalates.
Best Foods for Kidney Health
To recap, the best foods for kidney health are high in fiber, antioxidants, vitamins, and minerals, moderate in (preferably plant-based) protein, and low in phosphorus, fat, and sodium.
That leaves most, if not all, plant-based foods! Here are a few stellar kidney foods.
Lentils

Lentils are a safe, delicious, and versatile plant-based protein source that you can substitute for animal protein. Cooking lentils reduces their potassium and phosphorus levels to those recommended for CKD patients. Additionally, lentils are high in fiber and folate. Folate is important because research has found that amongst people with CKD, having normal levels of serum folate was associated with lower risk of mortality.
Flaxseeds

Flaxseeds are one of the foods for kidney health that can provide lots of valuable fiber, and are one of the richest sources of lignan precursors. Lignans are plant antioxidants that may play a role in glucose control and high blood pressure. Studies have found that flaxseed oil may reduce bone loss or shrinkage in hemodialysis patients.
Read our related article about ways to eat flaxseeds.
Blueberries

Blueberries may lower serum uric acid levels, which is a good thing if you’re not a fan of kidney stones. Furthermore, the anthocyanin antioxidants in blueberries can protect kidneys from oxidative stress and inflammation. Blueberries also appear to combat type 2 diabetes and heart disease by lowering their biomarkers (including the all-important blood pressure). Through all these and possibly other mechanisms, blueberries just might be a kidney’s best friend.
Leafy Greens

Low-oxalate leafy greens, a club that includes kale, collards, arugula, lettuce, and many others, provide necessary antioxidants, vitamins, and minerals, as well as being a good source of fiber.
Cauliflower

Cauliflower, like its cruciferous cousins, is a great source of sulforaphane, which in addition to being an anticancer powerhouse, may also help fight against oxidative damage caused by kidney disease. Sulforaphane also assists the liver in its job of detoxification of the blood, which takes some of the strain off the kidneys.
Cauliflower is also high in antioxidants, folate, fiber, and vitamin K1, which helps regulate your calcium balance and build strong teeth and bones — all of which are important when dealing with CKD.
Read our related article about creative ways to enjoy cauliflower.
Buckwheat

Buckwheat is a gluten-free whole grain that’s relatively low in potassium and phosphorus and may alleviate kidney problems in patients with type 2 diabetes. A good source of protein and fiber, buckwheat has been shown to protect kidneys and break up compounds that can harm them — in rodents, at least. (Our view on the use of animals in medical research is here.)
Grapes

Grapes, especially red ones, are rich sources of a compound called resveratrol that’s the subject of a lot of hype for its purported anti-aging properties. While the jury’s out on that one, it’s clear that resveratrol protects against CKD and its progression.
The flavonoids in grapes can benefit heart health and ameliorate the effects of type 2 diabetes, both of which can support kidney health. And grapes also contain quercetin, which helps maintain healthy blood vessels.
Chili Peppers

The more chili peppers you eat, the less likely you are to have kidney disease, at least according to this 2019 study of the eating habits and health status of over 8,000 Chinese adults. Eating chilis appears to decrease the risks of obesity and hypertension, both of which can increase the risk of CKD.
Another study from China showed that the enjoyment of spicy food enhanced the diner’s sensitivity to salt, which meant they needed and wanted less of it. This in turn lowered daily salt intake and blood pressure. And two compounds found in chili peppers, capsaicin and piperine, have been shown to improve kidney function.
Recipes with Kidney Healthy Foods
When it comes to healthy kidney function, focusing on fiber-dense foods (plants!) is key. Below you’ll find a tasty array of plant-based meals that contain tons of fiber, as well as other nutrients, to support healthy weight, blood pressure, insulin response, and bones. Consider your own unique needs when choosing foods for kidney health, making substitutions or omissions where necessary, since each individual’s dietary plan to meet kidney function goals can be different.
1. Blueberry Poppy Seed Pancakes

This one delicious breakfast boasts multiple kidney-friendly ingredients. Blueberry Poppy Seed Pancakes contain fiber-rich buckwheat flour. Flax meal provides lignans, which may help with blood pressure and blood sugar management. The blueberries are packed with anthocyanins, which are anti-inflammatory, helping support heart and kidney function. Of note, poppy seeds can be high in oxalates. One tablespoon of poppy seeds for four servings won’t put you over the oxalate level. However, if you’re concerned about kidney stones, simply omit the poppy seeds (the pancakes will still be delicious!).
2. Super Greens Salad with Bulgur and Lentils

Super Greens Salad includes healing, low-oxalate greens (kale and arugula), and provides a source of plant protein from lentils and pumpkin seeds. What’s more, there is plenty of fiber in this satisfying salad, found in the lentils, bulgur, pumpkin seeds, and greens. Super Greens Salad with Bulgur and Lentils can support kidney health, whether you’re simply trying to care for healthy kidneys or to prevent the progression of kidney failure.
3. Korean Cauliflower Tacos

Adding cruciferous vegetables like cauliflower to your plate may help fight against oxidative damage caused by kidney disease. Also, the detoxifying capabilities of sulforaphane may take some of the workload off of the kidneys (their job, after all, is pretty huge!). Take note, peanuts are high in phosphorus, so you may want to omit them if you’re watching your phosphorus intake. Also, if you’re watching sodium, consider adding crushed red pepper flakes in place of hot sauce to avoid sodium added to commercial hot sauce.
Keep Your Kidneys Healthy
Kidneys perform an important role in waste regulation, electrolyte balance, and the production of certain hormones. As the incidence of chronic kidney disease increases due to the increase in chronic diseases like type 2 diabetes and cardiovascular disease, it’s important to look at the lifestyle factors that may be impacting the kidneys. With chronic kidney disease, in particular, diet is one of the most vital lifestyle changes to consider — and a well-planned plant-based diet may be helpful in preventing or slowing the progression of the disease.
Tell us in the comments:
- What’s your favorite kidney-friendly food?
- What lifestyle change would most benefit your kidneys, and why?
- What else do you want to know about kidney health?
Feature Image: iStock.com/Lisovskaya



