When I was a teenager, I spent some time backpacking in Malaysia. One night, I woke to the sound of chewing close to my ear. Instantly full of adrenaline, I leapt to my feet and, clad only in my underwear, did my best warrior impression. Brandishing a pocketknife and a flashlight, I attempted to intimidate what I thought was some sort of monster that had invaded my hut.
Only after making a perfect fool of myself did I realize that my mortal foe was nothing more than a rat having a go at my water bottle lid. In short, I overreacted. Luckily, I didn’t injure myself or anyone else with my knife or my frantic flailing. (In fairness, it was a huge rat.)
There’s another way that many of us overreact — a way that we don’t have control over, and that can lead to much more serious consequences. I’m talking about allergies.
It surprised me, when I began researching for this article, how mystified scientists are about food allergies (and allergies in general). Basically, an allergy is when your body reacts to exposure of an otherwise harmless substance as if it were toxic. We don’t know what causes food allergies, or why so many more people have them now than even 30 years ago.
In the United States today, for example, recognized food allergies affect approximately 7.6% of children and 10.8% of adults. And some of the people with food allergies either don’t know they have them or haven’t reported them. So the number of people suffering from some degree of allergic reaction to otherwise perfectly safe foods is probably quite a bit higher. Most of us know someone with a food allergy (or you may have one yourself).
Allergies can be not only a real pain, but potentially life-threatening as well. And since the most common allergens are, well, common, they’re often hard to avoid and can hide in packaged foods, restaurant meals, and in the recipes of friends and neighbors.
So what is a food allergy? What do we know about the biological pathways triggered when someone eats a food they’re allergic to? What are the most common types? How do they develop in the first place? And once you’ve got one, what can you do about it?
What is a Food Allergy?

A food allergy is an immune response to a particular protein in a food. To qualify as an allergen, the food in question must be normally harmless for most people. That is, you can’t be allergic to antifreeze, because antifreeze is straight-up toxic. An allergy is basically your immune system going overboard in its “quality control” mission, rejecting substances that otherwise would not be a problem.
Here’s what happens when you consume a food you’re allergic to. Initially, your immune system produces antibodies — summoned to the substance in question — which are meant to surround, neutralize, destroy, and eliminate it. This ability of your immune system is normally a good thing; without it you wouldn’t be able to fight off a cold or an infection, and pretty much everything could potentially kill you. In the case of a food allergy, however, it’s like emptying the fire extinguisher every time you light a candle. (You probably wouldn’t last long as a server in a romantic restaurant.)
The antibodies travel to cells that release various chemicals that cause allergic symptoms. Most often, these symptoms occur in the nose, lungs, throat, sinuses, ears, stomach lining, or on the skin. (You can find out more about symptoms on the website of the American Academy of Allergy, Asthma, and Immunology, which is at aaaai.org, and which you should definitely pronounce “Aaaayeee.”)
Allergies that can be immediately life-threatening typically manifest within minutes of eating the trigger food or allergen. There are two basic allergy pathways. The one that acts quickly involves an antibody called immunoglobulin E (IgE). The other, non-IgE, pathway can take longer — up to several hours or in some cases even longer — to act.
Allergies differ significantly from food sensitivities and intolerances. Food sensitivities typically trigger a subtle immune response (including fatigue, joint pain, rashes, and so on). And with a food intolerance, the effects are often exclusively gastrointestinal in nature.
Food Allergy Symptoms
A major allergic reaction to a food may cause a life-threatening condition called anaphylaxis. The word comes from the Greek “ana” (upward) and “phylax” (guardian, protector). You can think of anaphylaxis as trying to swat a fly with a sledgehammer. The fly will probably be fine, but the walls and windows are in trouble.
There’s an awful lot of this sledgehammering going on in the world. In the US, about 1 in 50 people experience anaphylaxis from one cause or another (not just food). Food allergy symptoms typically start within 5–30 minutes, or sometimes up to an hour, of coming into contact with the allergen.
Food allergy symptoms can include:
- Red rash, with hives/welts, that is usually itchy
- Swollen throat or other areas of the body
- Wheezing, trouble breathing, or trouble swallowing
- Tingling in hands and feet
- Severe lowering of blood pressure and shock (“anaphylactic shock”)
- Loss of consciousness
A friend’s anaphylactic reaction (to an unwashed, unpeeled mango) included most of the above, along with a powerful panic attack and the certainty that he was dying. (And without the rapid medical attention that he received, he probably would have.)
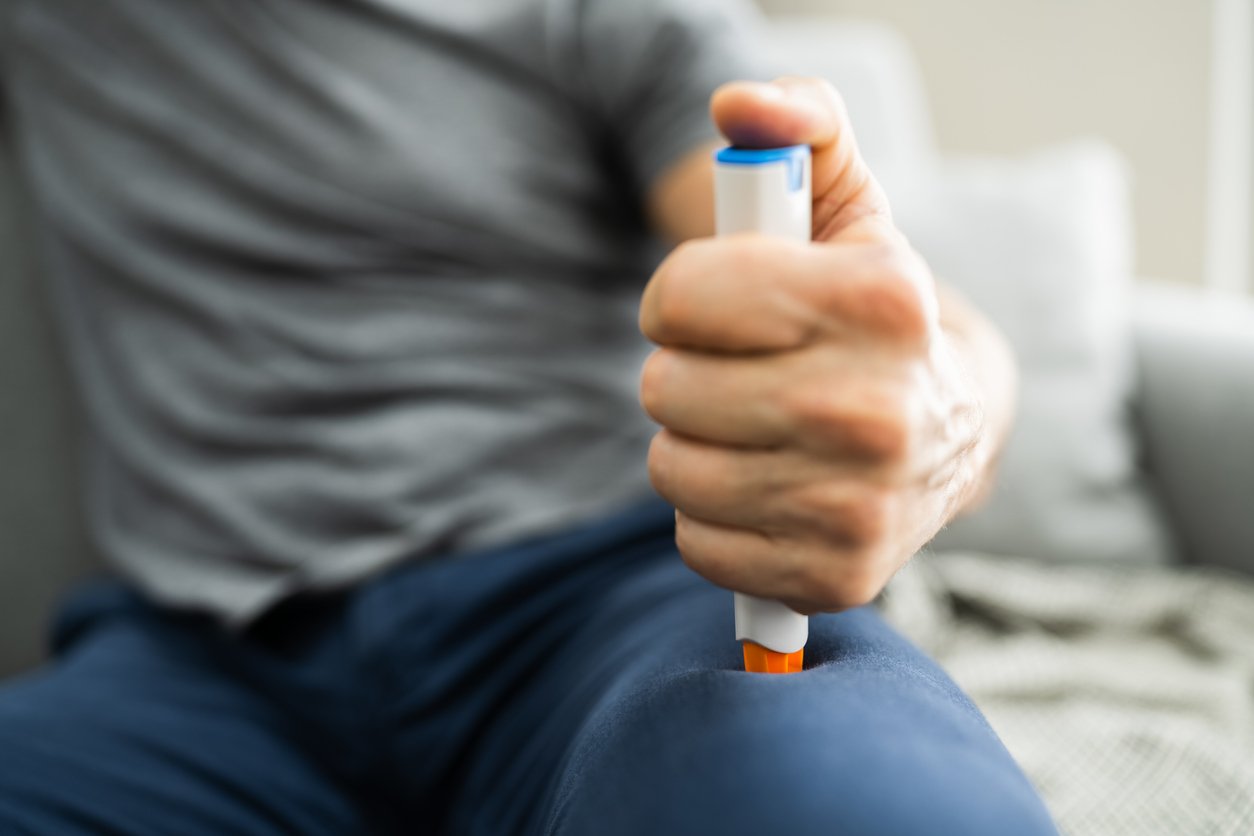
Anaphylaxis is a medical emergency, but it can be treated with an epinephrine autoinjector (the best-known brand is EpiPen) until emergency medical care can be given.
But not all allergic reactions are that severe. Non-anaphylactic reactions may include:
- Hives or red, itchy skin
- Stuffy or itchy nose, sneezing, or itchy, teary eyes
- Swelling
- Gastrointestinal issues like diarrhea, indigestion, nausea, passing excessive amounts of gas, or vomiting
Who Can Have a Food Allergy?
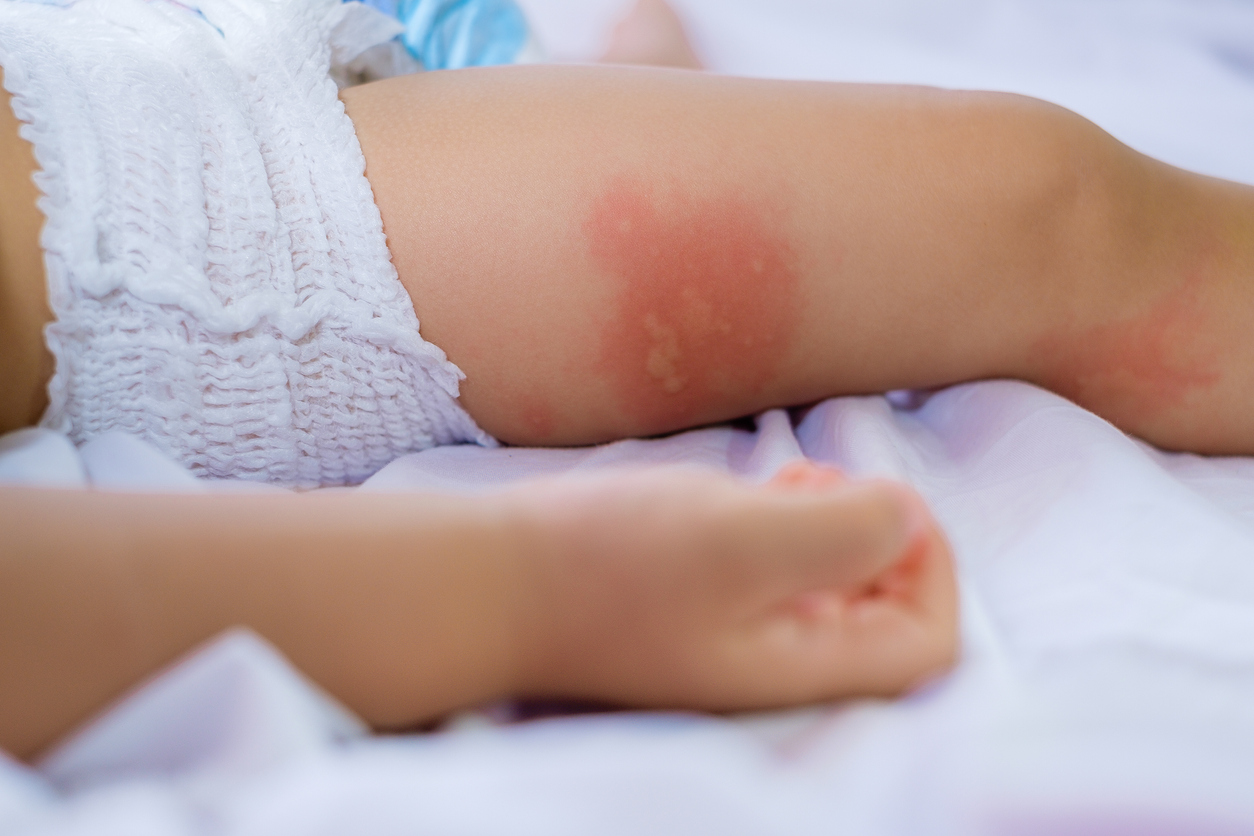
Food allergies can affect both children and adults, although they are more common in children. We don’t understand why or how, but people can sometimes outgrow their childhood food allergies. For example, many eventually shed childhood allergies to cow’s milk, eggs, soy, and wheat, even if they have a history of severe reactions. Other food allergies tend to persist through adulthood, such as peanut, tree nut, fish, and shellfish allergies. And some adults develop new allergies throughout their lives.
Major Food Allergens

Because an allergy is an overreaction of the immune system, pretty much any food could theoretically trigger an allergic response. In practice, though, there are a handful of common food allergy triggers (which can vary slightly from one geographic region to another).
In the US and UK, eight major foods account for 90% of allergic reactions:
- Milk
- Tree Nuts
- Eggs
- Peanuts
- Fish
- Wheat
- Shellfish (including mollusks and crustaceans)
- Soybeans
You know how a few years ago, Pluto was demoted from being a planet when astronomers discovered a bunch of similarly sized objects that are also revolving around the sun? Well, immunologists in the US have recently added a new food to the list of major food allergens. On April 23, 2021, the Food Allergy Safety, Treatment, Education, and Research (FASTER) Act was signed into law, declaring sesame as the ninth major food allergen recognized by the US government. This change went into effect on January 1, 2023, and food manufacturers are now required to list sesame-containing ingredients on all food packaging either next to an ingredient in parenthesis or in a “Contains” statement after the list of ingredients.
Canada and the European Union (EU) include celery, mustard, sulfur dioxide, and sulfites in their list of common allergens, while the EU adds the lupin bean (a legume relative of the peanut). A 2015 study found that common allergens in Latin American and subtropical regions include chili pepper, tomato, banana, guava, and mango.
Food Additive Allergies
It’s not just plant or animal ingredients that can trigger an allergic reaction, however — food additives can, too. This includes fully synthetic additives like FD&C Yellow No. 5 (aka tartrazine), the preservatives BHA and BHT, and the sweetener aspartame. It also includes natural additives such as lecithin and gums, and colorings such as carmine (a red hue derived from the carapace of certain scale insects) and annatto (an orange-red colorant made from the seeds of a tropical tree).
Rare Food Allergies
Other types of food allergies exist that are currently quite rare, so I won’t go into them here. If you want to dive deeper into the topic, a good resource is the aaaai.org website I mentioned earlier. You can find articles on Oral Allergy Syndrome (triggered by some fruits and vegetables), Food-Protein Induced Enterocolitis Syndrome (in which a baby has an allergic reaction to early exposure to solid food), and Eosinophilic Esophagitis (a tricky one to diagnose because symptoms can take a while to appear after eating the trigger food).
The one relatively rare allergy that I will mention, partly because it appears to be getting more prevalent every year, is alpha-gal. Alpha-gal an allergy to galactose-alpha-1,3-galactose — which isn’t the name of a TV show about outer space, but rather one of the rare carbohydrates found in mammalian meat. The allergy appears to be triggered by a bite from the lone star tick and makes it very unpleasant for the sufferer to eat beef, lamb, pork, venison, and other meats and animal-derived products like dairy and gelatin. Many people are unaware that they have this condition since, unlike most allergic reactions, alpha-gal symptoms typically take 2–6 hours to appear.
Food Allergy Testing
If you’ve had an allergic reaction to food, or suspect a food allergy, an allergist can help clarify your needs. You can devise a treatment plan, and be prepared with knowledge and supplies in case of anaphylaxis.
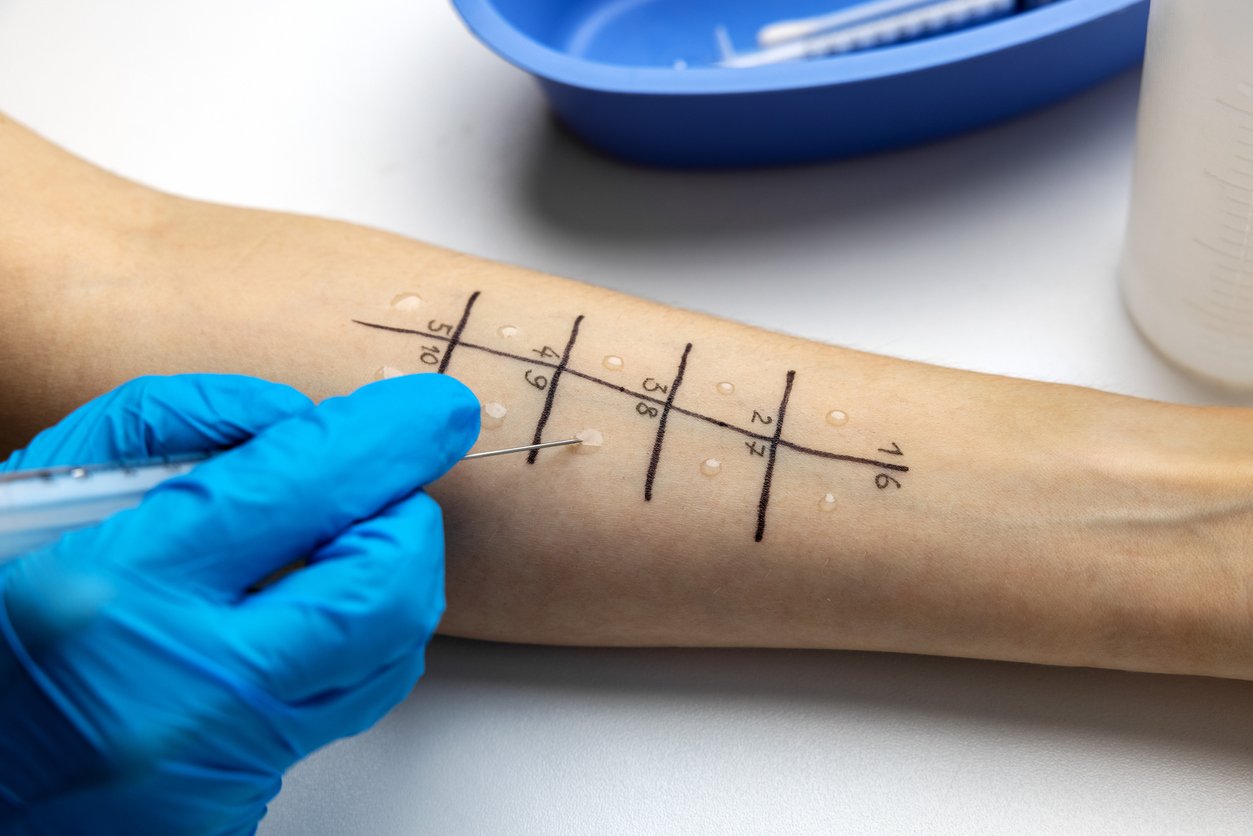
The allergist will probably start you off with a skin prick test, in which a small amount of extract made from the suspected allergenic food is placed directly on your skin, typically on the back or arm. If a raised bump or small hive develops within 20 minutes, that’s considered a positive indication of an allergy.
The good news about this test is, if you don’t react, you most likely aren’t allergic to that food. The less-than-good news is, a reaction isn’t conclusive, as the test has a high false positive rate (in fact, over half of positive reactions are errors). Allergists, therefore, use the skin prick test mainly to rule foods out, and to create a list of possible allergens to investigate further.
Food Allergy Panel
Another diagnostic for allergies is a food allergy panel, which is a type of blood test. It looks for IgEs in the blood that may have formed in response to particular foods. But just because the IgEs are present, it doesn’t mean that there’s an allergy. For that reason, this test also has a high false positive rate.
Oral Food Challenge
The most reliable test for food allergies is the oral food challenge. It’s what it sounds like: you eat a food and see what happens. The test is conducted under strict medical supervision and involves feeding the patient tiny amounts of the suspected trigger food in increasing doses over a period of time. Then the patient is observed for a few hours to see if a reaction occurs.
Elimination Diet for Food Allergies
For less serious allergies, you can perform a rough DIY version of the oral food challenge known as an elimination diet. You take your list of positives from the skin prick or food allergy panel (or simply foods you suspect might be problems for you) and eliminate them all from your diet for a couple of weeks or more. If you get relief from all allergic symptoms, you know the culprit or culprits are in there somewhere.
Then you slowly add foods back into your diet, one at a time, to see if the symptoms return. Make sure you go slowly and journal or chart the whole process, including the steps you take and the results you experience, so you can be as objective as possible. Sharing this data with your health care team can aid them in guiding you to improved health.
Potential Causes of Food Allergies

We’ve seen the prevalence of food allergies skyrocket over the past 30 years, but we’re not yet sure what that means. The internet is full of theories, ranging from the plausible to the frankly absurd, but it will take much more research to eliminate the red herrings (unless, of course, you’re allergic to red herrings).
One popular theory on what causes food allergies is the so-called “hygiene hypothesis.” This theory argues that by growing up in increasingly clean and “antibacterial” environments, we’re essentially coddling our immune systems so they don’t have the opportunity to figure out what’s harmful and what’s not.
And there is some solid evidence to support this theory. We know that children growing up in larger households have a lower incidence of allergic disease compared with children from smaller families. Environmental exposures early in life, such as growing up on a farm and living with companion animals, are also associated with a diverse bacterial experience and reduced risk of allergic sensitization. Children who live with cats and dogs when they are infants are less likely to develop allergies later in childhood.
For a while, researchers thought that it was exposure to various parasites that made it difficult for the immune system to distinguish between harmful and harmless substances. The problem is, most parasites were eliminated from the developed world a while ago, and yet rates of allergy continue to rise dramatically. So something else must be going on.
The Role of the Microbiome in Food Allergies
In the last decade, science has begun to unlock the mystery of the microbiome, those teeming populations of microorganisms that live in and on us, in the soil, and in pretty much every organism on the planet. One explanation for the fact that dirty childhoods (within reason) tend to create fewer allergy-prone adults posits that early and prolonged exposure to a variety of microbes helps to cultivate a healthy immune system.
We know that IgE-mediated food allergies have been associated with both immune dysregulation and impaired gut. And 70% of the immune system resides in the gut. The argument now goes, dysregulation of the microbiome, in ourselves and in our environment, causes the immune system to get confused and overreact to innocuous substances as if they’re lethal toxins.
People who live in urbanized environments experience higher rates of allergy, and they also suffer disproportionately from asthma and atopic dermatitis (aka eczema). There’s a strong association between having eczema and having one or more food allergy. And the microbiome is looking more and more like the smoking gun (or the dripping fire extinguisher, sitting empty over a candle, if you prefer that metaphor).
A Fiber Deficit
So what’s harming our microbiome? For one thing, most people in developed countries don’t get enough fiber in their diets. That fiber deficit means that they don’t produce enough short chain fatty acids (SCFAs), which are supposed to be metabolized by the bacteria that ferment nondigestible fiber in the large intestine.
SCFAs are essential for maintaining immune homeostasis in the gut by regulating protective and inflammatory responses. Test-tube and clinical studies have validated the importance of SCFAs in relation to food allergies. If we want to prevent food allergies in children, one approach is to increase the amount and variety of fiber in their diets.
Junk Food and Fast Food
Another source of microbiome damage may be junk and fast food. In one study at the University of Naples ‘Federico II, researchers found that children with food allergies, and children who eat a lot of junk food, both had increased levels of molecules called advanced glycation end-products (AGEs). Researchers found that children with food allergies consumed approximately 20–40% more junk food (on average) compared to healthy controls. It could be that AGEs are toxic to immune cells, and could disrupt the gut mucosal barrier, allowing toxins and allergens to come into contact with deeper body tissues.
Environmental Toxins
Other changes in our food environment, and our environment in general, may also be wreaking havoc on our microbiomes. These include increased exposure to chemical additives, preservatives, and colorings, as well as plastics, pesticides (specifically glyphosate, one of the active ingredients in Monsanto-Bayer’s Roundup, and potentially a major driver of gluten allergies), and antibiotics used in industrialized animal agriculture.
Early Childhood Influences
Other factors are more individualized, such as being born by C-section rather than vaginal delivery (since a major way the mother transfers her microbiome to her newborn is via the birth canal), as well as the introduction of solid foods too early in infancy. Early antibiotic exposure may also contribute to microbiome dysregulation (it’s right there in the word antibiotic: “against life”). Finally, waiting too long to introduce babies to potentially allergenic foods seems to set the table for later food allergies. The latest recommendation is to start exposing children to common allergenic foods between six months and one year.
What to Do if You Have a Food Allergy

While some childhood food allergies abate by adulthood, there’s no known food allergy cure. But there are things you can do to diminish their impact on your life.
The most important is also the most obvious: avoid foods you’re allergic to. Even if it’s a healthy food that we typically recommend as part of a healthy diet, your allergy trumps generalized guidance.
Read Food Labels Carefully
Read food labels carefully, especially if you’re unfamiliar with a particular packaged food. Certain common food allergens like soy, eggs, wheat, and nuts, are very prevalent in our industrialized food supply.
Processed foods in particular are likely to be trouble. That’s partly due to all the food additives they contain, and partly because they tend to include hidden proteins from milk, eggs, and soybeans — both to enhance flavor and to increase the protein content so they can brag about it on the label.
Pay special attention to sauces and dips, as many of these contain peanuts and/or tree nut products for texture and flavor.
Use Caution at Restaurants
If you eat out, let restaurant staff know about your allergies. Don’t worry about bothering them or making a scene. Compared to you going into full-blown anaphylaxis during dessert, asking about peanuts and eggs in advance is actually quite considerate. Believe me, if a server or cook has ever witnessed a customer having an allergic reaction in their establishment, they never want to have that happen again. You can download an official-looking Chef Card from FoodAllergy.org (it’s available in multiple languages), to fill out and carry in your wallet, to make sure you get the staff’s attention.
Keep Medication On Hand
Prevention is key, but you also need to have a plan in case an allergen slips by, and you start reacting. If you’re prone to severe reactions — or if your reactions are becoming more and more severe over time — carry an EpiPen or an over-the-counter antihistamine (such as Benadryl) with you at all times.
Children with peanut allergies can now also access an oral immunotherapy called Palforzia, which the US FDA approved in January of 2020.
Eat More Fiber
More generally, you want to give your immune system its best chance to stay balanced and appropriately responsive. One way is to eat whole foods and avoid processed foods. And while a fiber-rich plant-based diet can’t cure food allergies, it may be able to help.
As we’ve seen, lack of fiber may play a role in the development of food allergies. It turns out that introducing more fiber in the diet may help with symptoms of allergic reactions. Studies show a high-fiber diet created significant differences among gut bacteria, immune system cells, and allergic reactions to food compared to a low-fiber diet.
Did you know that every fruit and vegetable has its own type of fiber? Consuming lots of fiber and lots of different kinds of fruits and veggies keeps “good” bacteria in the gut happy, which in turn helps keep the lining of the gut healthy, which in turn may lower the risk of allergic reactions to food.
Not only do fruits and vegetables provide fiber, they also contribute antioxidants that help your microbiome thrive. Allergic conditions are characterized by inflammation, and antioxidants combat inflammation. Epidemiological studies show that the greater the amount of antioxidants in the diet, the less frequent and severe are the symptoms of allergic reactions.
Choose Healthy Allergen Alternatives
Finally, substitute wisely. Choose healthy alternatives to foods you are allergic to. Instead of tree nuts, try seeds. If you’re allergic to sesame seeds, try sunflower or flax seeds. In place of soybeans, experiment with other beans, peas, or lentils. Find a plant-based alternative to dairy foods. Replace eggs with tofu or another plant-based alternative. And instead of fish or shellfish, try plant-based, omega-3-rich foods like walnuts, chia seeds, and flax seeds, plant-based sources of protein, or algae and seaweed. And if you’re allergic to wheat, or to gluten in general, there are plenty of gluten-free whole grains and bread mixes on the market for you to sample.
Allergen-Free Recipes
Having a food allergy (or several) does not mean you need to miss out on flavors, textures, or nutrients. There are over 20,000 edible species of plants in the world so, technically, there should be lots of other options. Instead of passing over a recipe that contains ingredients that don’t agree with you, try searching for ingredient substitutions. This opens up recipe possibilities, and also opportunities to try new foods and get a variety of nutrients. Try the recipes below that offer a wide array of ingredients that promote gut health. They are free of common allergens and substitutions are offered where allergens could be a possibility.
1. Ocean’s Savory Oatmeal

Looking to enjoy a nutrient-dense breakfast that will leave you feeling full, nourished, and energetic? Try my savory (Instant Pot) oatmeal! Feel good knowing that this morning meal boasts abundant ingredients — turmeric, kale, oats, garlic, and more! — that support optimal health. If you have a gluten allergy, be sure to choose certified gluten-free oats. If you prefer to avoid oats altogether, try this recipe with naturally gluten-free quinoa, millet, or amaranth instead. If soy is an issue for you, then choose coconut aminos in place of tamari. Getting creative with substitutions means you’re able to try a variety of recipes that are customizable to your own individual needs!
2. Instant Pot Wild Rice and Veggie Soup

Enjoying a wide range of allergy-friendly and fiber-rich plant foods fuels the good bacteria in your gut, creating microbial symbiosis. Plus, you benefit from many more nutrients since each plant food brings its own set of vitamins, minerals, and phytonutrients. Instant Pot Wild Rice and Veggie Soup has lots of flavorful and nutritious ingredients, and comes together quickly! (P.S. It can also be made on the stovetop or in the slow cooker.)
3. Cauliflower Squash Cheese Sauce

We’re pretty sure that you will no longer feel the need for or even want dairy-based cheese sauce after you make and try this plant-based version. It’s creamy, flavorful, and chock-full of fiber. Unlike dairy, which has zero fiber (and is prone to triggering inflammation and allergic reactions), this cheesy sauce can support a healthy gut, which in turn supports a healthy immune system. Enjoy this on top of tacos, as a legume pasta sauce, or drizzled over your favorite steamed veggies! (Note: If you’re allergic to soy, be sure to opt for the chickpea miso.)
Living with Food Allergies
Food allergies are increasingly prevalent worldwide, in both adults and children. While many different foods can trigger allergic reactions, fewer than a dozen are the most common allergens. Although we don’t know the precise cause of food allergies yet, there’s increasing evidence that they start in the gut, where most of the immune system lives and works.
While we don’t know of any complete cure for allergies, there are things you can do to help, like eating a whole foods, plant-powered diet free of processed foods. If you suspect you have a food allergy, you may want to check with your health care professional about getting tested. And if you do have a food allergy, be sure to avoid that food and have an emergency treatment plan ready to go in case of an allergic reaction.
Tell us in the comments:
- Have you been diagnosed with any food allergies? If so, what foods do you avoid?
- If you suspect that you may have an undiagnosed food allergy, what steps will you take to check it out?
- Even if you don’t have a food allergy, which of the recipes we shared in this article do you want to try?
Feature Image: iStock.com/AndreyPopov

